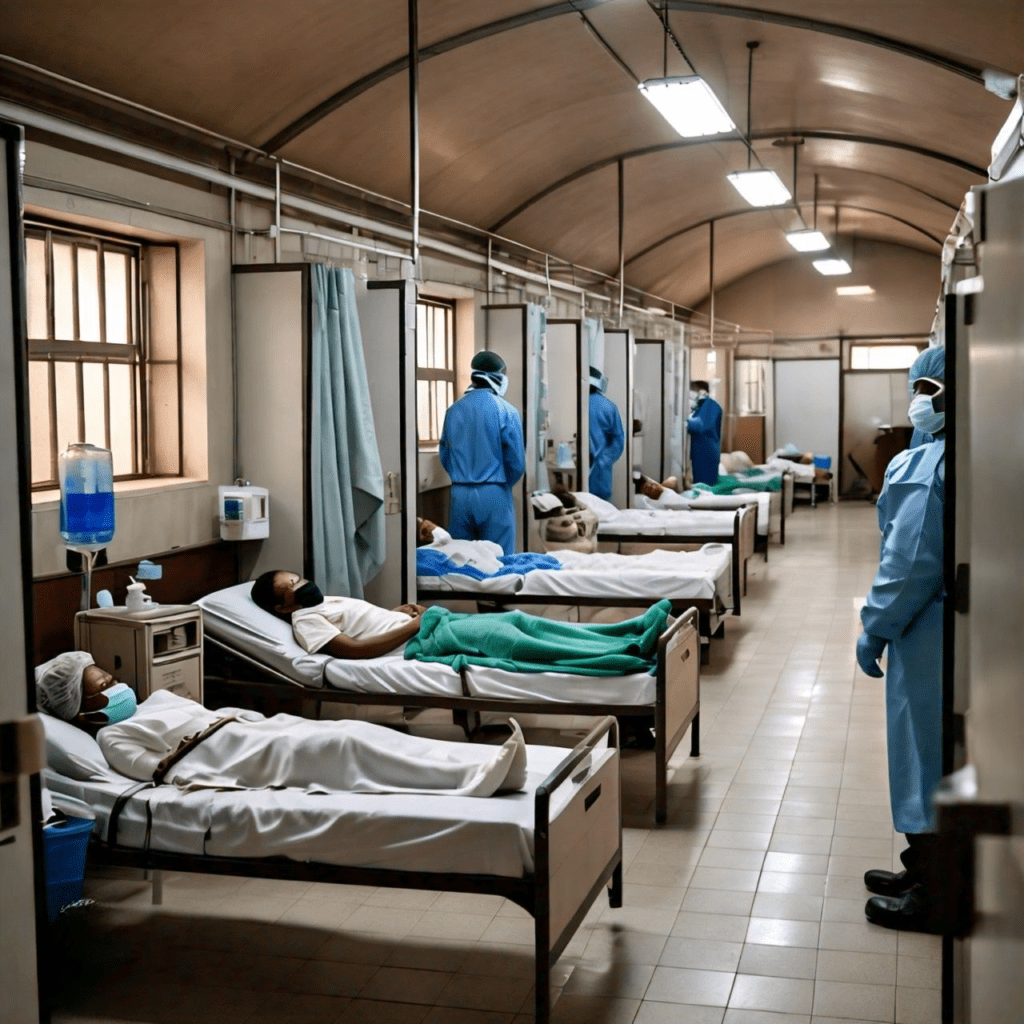
During the COVID-19 pandemic, governments the world over sought to limit its spread through the establishment of COVID-19 treatment centres (CTC) – certainly at the start of the pandemic, but also during peak waves. It was in these centres that persons infected with COVID-19 were mostly interned and taken care of. In most cases, these patients were kept there against their will, without companion (family, friends, etc.) as the main aim was to contain the crisis and curb the spread of the pandemic. In this article, we zoom in on Covid-19 care centres in Benin and the experiences of patients (survivors) in these centres, during their stay and after being discharged.
The findings shared here emanate from the research project “Rectifying the Effects of COVID-19 on Vulnerable populations in West Africa: a Research-action (RECOVER)” which ran from November 2020 to February 2024. RECOVER was funded by IDRC, with technical support from ITM, Antwerp. In this blog, we share some insights from a content analysis of interviews done with five persons, both health workers and patients, interned and discharged from the CTC at Allada, a southern town in Benin. All interviews took place in 2022. Interviewees had been interned during the first (2020) or the third wave (2021) of the pandemic. In total, Benin has recorded 4 waves of COVID-19, with the highest number of cases during the second wave.
Conditions during their stay
How about the cost first of all? In the CTC, biological and X-ray examinations, as well as catering and hospitalisation costs, were paid for by the government. However, products and medicines for illnesses and conditions not related to COVID-19 were paid for directly by the patients and/or their parents, certainly during the latest waves (as compared to the first when all were free of charge). All persons interviewed said that their experience of care could (and should) have been more humane. Due to their internment, these people were no longer free to pursue income-generating activities, or access their accounts to withdraw money, yet they still had to (i) manage certain pathologies that were either known or diagnosed for the first time during their stay in the CTC, and/or (ii) assume their social responsibilities as parents. They managed these comorbidities with the support of family members who sent financial support to the managers of the facility through mobile money transfers. Interviewees saw their stay in the CTC as resembling a prison because they were deprived of their freedom of movement and contact with their families.
In addition, they could not have access to the CTC courtyard when their state of health improved. They were forced to wash dirty clothes and lay them out in the hospitalisation room. Their only leisure activities were watching television, reading, and playing games on their phones/tablets. In a context where care remained essentially biomedical (without foreseeing mental health care even if needed), these living conditions increased the negative impact on their mental health and wellbeing. Fortunately, the absence of patient carers triggered other forms of psychosocial support between patients. Indeed, patients suffering from less severe forms of the disease (who were not on respiratory assistance) acted as nursemaids for others.
Clearly, the care experience of these patients would have been better if the cost of treatment of co-morbidities had been borne by the government to ease the financial burdens of the interned. Also, no doubt patients’ experience of care would have been better if care centres had also provided some “social facilities”, like a gymnasium, a swimming pool, or a library. All of these would have improved considerably the quality of their lives during the quarantine.
Burials & reintegration
As we all recall from the pandemic, not everybody survived, sadly. People who died at such emergency centres were often buried under supervision by designated health professionals at selected burial grounds. Their families had little or no control over how and where they were buried. The corpse of a person who died from COVID-19 could not remain in a care centre for more than 24 hours. And so customs, traditions, and family preferences regarding burials were often relegated to the background. All this traumatized bereaved relations, and created further anxiety, stress and fear among the citizenry but also among patients still staying at the CTC.
Last but not least, there’s the reintegration of patients who survived into their various communities. The persons interviewed revealed that no psychological support was available for those being reintegrated into communities. Just one example perhaps of the reintegration problems: during the stay of one of the health workers as a patient, a national television report showed his face. In our interview, he claimed to have experienced stigmatisation once back in the community – in spite of having a certificate of recovery. Obviously, there is a need for increased efforts to support the social, professional, and economic reintegration of survivors in communities.
As pandemic agreement negotiations are still ongoing in Geneva, let’s hope such an agreement will also show sufficient attention for human rights of patients in future pandemics, and for the reintegration of survivors in their communities.